💌 Dear all 💌 ,
I hope you’re doing well, and even if the times are still challenging (another lockdown for many, pandemic stress etc.), let’s recall that November is the month of Gratitude. And this month, we have had the best news of the year so far (hopefully with more to come soon!): we have encouraging news about Covid vaccines (although many questions are yet to be answered) and the USA will have a new president. Each of us surely has other good news as well, but we can already be grateful together for those two! And do not forget about enjoying the nature, the colours are amazing these days!
Let’s now have a look at a few research papers that can potentially help us to have better health.
Melatonin & Covid-19
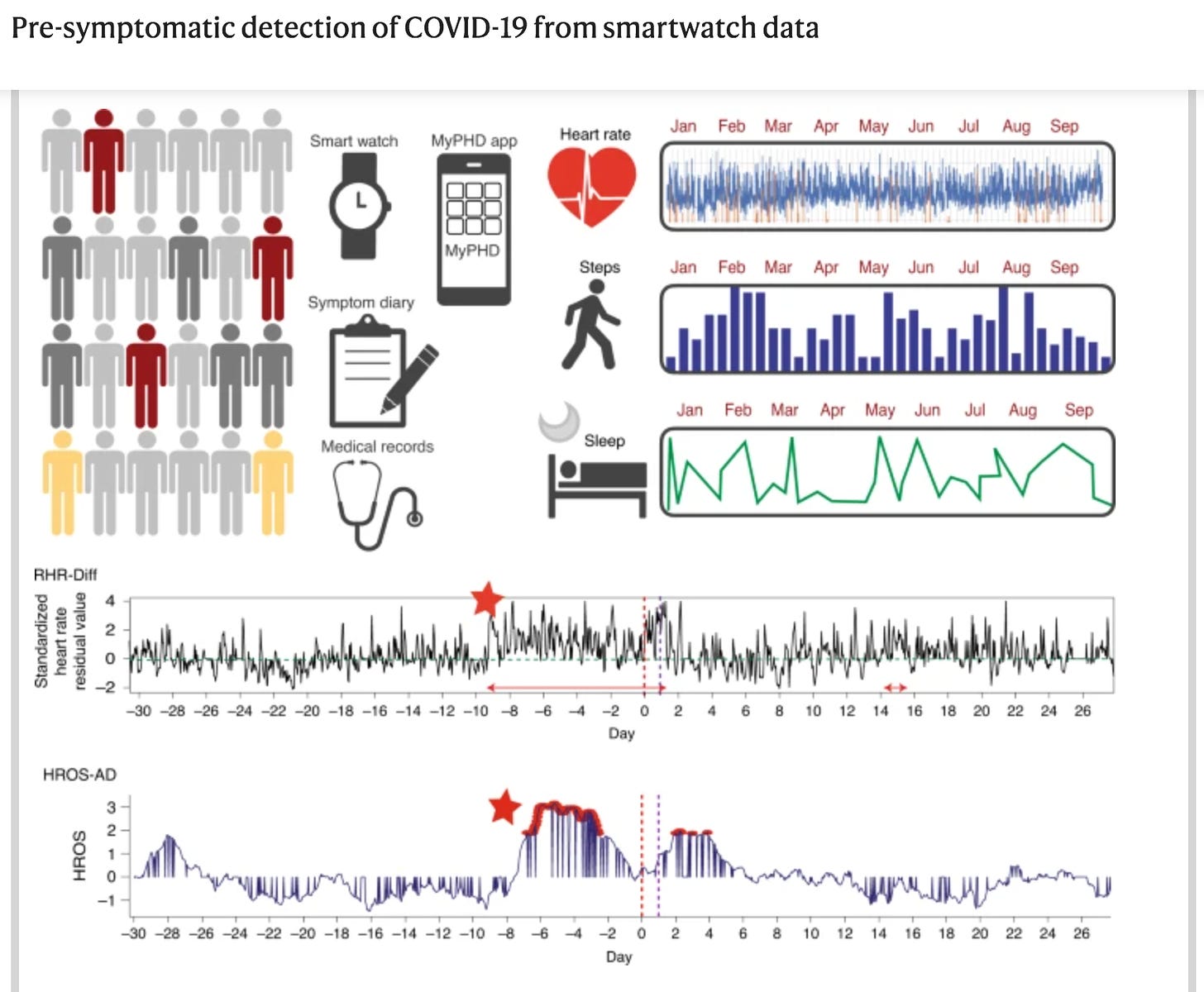
Pre-symptomatic detection of COVID-19 from smartwatch data
Persistent fatigue after COVID-19 common and independent of disease severity
MELATONIN & COVID-19
One of the things we’ve learned about Covid-19 so far is that it is a systemic disease. In other words, although the respiratory symptoms are the most predominant and lungs being commonly affected, the virus impacts multiple cell types, tissues and organs. So “knowledge of the complex interplays between the virus and other diseases is key to understanding COVID-19-related complications and identifying repurposable drugs," said Dr. Cheng, one of the author of this recent study about Covid-19.
Researchers analysed data from large-scale electronic health records from Cleveland Clinic patients to identify clinical manifestations and pathologies shared between COVID-19 and other diseases. Specifically, they measured the proximity between host genes/proteins and those associated with 64 other diseases across several disease categories (malignant cancer and autoimmune, cardiovascular, metabolic, neurological and pulmonary diseases), where closer proximity indicates a higher likelihood of pathological associations between the diseases.
This ‘network medicine approach’ using omics technologies allowed the researchers to further identify 34 drugs as repurposing candidates for Covid-19, with melatonin chief among them. Melatonin usage was associated with a nearly 30 percent reduced likelihood of testing positive for SARS-CoV-2 (the virus that causes COVID-19) after adjusting for age, race, smoking history and various disease comorbidities. Notably, the reduced likelihood of testing positive for the virus increased from 30 to 52 percent for African Americans when adjusted for the same variables.
"It is very important to note these findings do not suggest people should start to take melatonin without consulting their physician," said Feixiong Cheng, Ph.D., assistant staff in Cleveland Clinic's Genomic Medicine Institute and lead author on the study. "Large-scale observational studies and randomized controlled trials are critical to validate the clinical benefit of melatonin for patients with COVID-19, but we are excited about the associations put forth in this study and the opportunity to further explore them”.
A few facts about melatonin:
What is it? A “sleep hormone'' but also the most powerful antioxidant produced by the human body.
Can you increase your melatonin level through your lifestyle? Yes! Firstly, by having enough daily light exposure (at least 20 min/day) and having a dark environment for your nightly sleep (no lights at night in your bedroom and no blue light -i.e. screens - for a few hours before going to bed). Also, there are some foods that can help to increase your melatonin levels. The foods richest in melatonin are tart cherries, grapes, and strawberries. Other foods rich in melatonin are eggs, fish, black rice, mushrooms etc. There’s a nice study about the topic here.
Can you have Melatonin medication? Yes, if it is prescribed by your doctor and if your test indicates that you need treatment.
Can you get melatonin over the counter? Firstly, it is really important to have medical advice even if you can buy it without prescription. So yes, you can get Melatonin over the counter in some countries (France, USA) while in others you cannot (UK) or you can only get it with some restrictions (small dosage products are available in Germany and Belgium, for example).
Can you test for it? Yes, in saliva or 24h urines. If you have sleep problems, you should check your melatonin levels with your doctor, among other things (ideally, the cortisol rhythm as well as the stress hormone). Ask your doctor or ping me.
FATIGUE & COVID-19
You may have heard about ‘long Covid’- people having symptoms persist for months after having the disease, with fatigue being one of the most common. A recent study from the Department of Infectious Diseases, St James’s Hospital, Dublin, Ireland found that ‘persistent fatigue following SARS-CoV-2 infection is common and independent of severity of initial infection’. During a median follow up of 10 weeks, there was significant burden fatigue with 50 % of the patient cohort reporting severe fatigue while as much as 30% of the participants in the study couldn’t return to work.
“A lengthy post-infection fatigue burden will impair quality of life and will have a significant impact on individuals, employers and healthcare systems. These findings should be used to inform management strategies for convalescent patients and allow intervention to occur in a timely manner,” say the authors of the study.
So, if you have recently had Covid and still feel tired, it’s not just in your head. Ask for help from your doctor to have full support.
WEARABLES FOR COVID-19
Consumer wearable devices like smartwatches are already very popular to measure many physiological parameters, such as heart rate, skin temperature and sleep patterns. That continuous measurement of vital signs can be used to monitor the onset of infectious diseases.
A team of researchers from Stanford University investigated the use of wearable devices for the early detection of COVID-19 in a retrospective manner. Using heart rate and steps data from a large cohort of 5,262 individuals, they have shown that heart rate signals from fitness trackers can be used to retrospectively detect COVID-19 infection well in advance of symptom onset (offline detection).
“We analysed physiological and activity data from 32 individuals infected with COVID-19, identified from a cohort of nearly 5,300 participants, and found that 26 of them (81%) had alterations in their heart rate, number of daily steps or time asleep. Of the 25 cases of COVID-19 with detected physiological alterations for which we had symptom information, 22 were detected before (or at) symptom onset, with four cases detected at least nine days earlier.
Using retrospective smartwatch data, we show that 63% of the COVID-19 cases could have been detected before symptom onset in real time via a two-tiered warning system based on the occurrence of extreme elevations in resting heart rate relative to the individual baseline.”
MISCELLANEOUS
Personalised diabetes care- January AI
Blood pressure- continuous measurements device
Gut bacteria- inflammation- Alzheimer- new discoveries
Fermented food at your door (available in the UK):
Until next time, stay healthy and take care of yourself and your loved ones! Please do not hesitate to contact me at lavinia@drionita.com
Love your health,
Lavinia💖Dr Lavinia Ionita
Functional Medicine doctor | founder of Akesio
Important note:
The content of this Newsletter is not a medical advice. If you have any health issues, please look for medical assistance without any further delay from your healthcare provider .